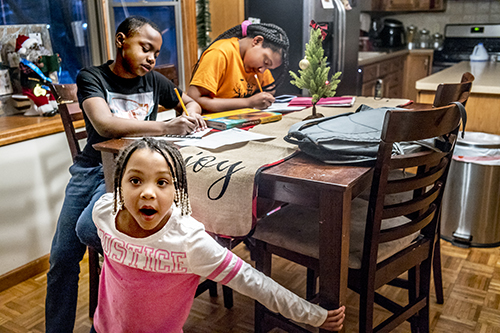
Liberty Sommerville, 4, was born in France. Her siblings were born in America. The different systems of healthcare illustrate dramatic gaps in U.S. coverages. (PHOTO BY DAVID ZALAZNIK FOR COMMUNITY WORD)
Brooke Sommerville gave birth to three children in Peoria. Then her husband, professional basketball player Marcellus Sommerville, was recruited to play professionally in France.
The family moved to France, and Brooke didn’t know what to expect when she became pregnant with her fourth child.
She loved her doctor in America and wondered if she should fly home for the birth. She didn’t. She remained in France and her experience was wonderful, supportive and eye-opening.
The differences in maternal healthcare and newborn care were dramatic. Liberty Sommerville, now 4, was born in France.
“I had a lot more doctor visits leading up to the birth, and once I had Liberty, my stay in the hospital was a lot longer,” Brooke Sommerville said. “Liberty was a C-section. It was really smooth and the incision was glued rather than stitched.”
Sommerville’s first child had also been delivered by Cesarean-section. Her doctor in France didn’t like the scar from that delivery. He made the incision for Liberty in a way that minimized the previous scar. The healing process by gluing was faster and with less pain than the stitches.
“I felt I could go home in two days, but in France they keep you longer in the hospital,” Sommerville said.
The extended stay meant more sleep and no demands from a busy household filled with three other children.
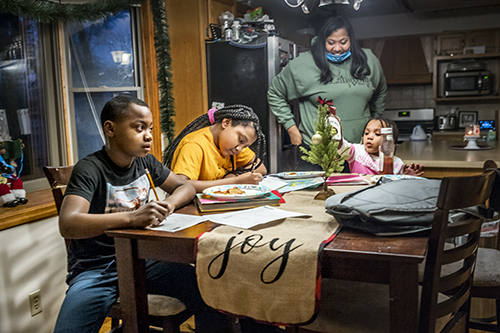
Brooke Sommerville oversees children Lawson and Londyn doing their school homework at the kitchen table while she and Liberty set the table for a snack. Liberty, 4, was born in France. (PHOTO BY DAVID ZALAZNIK FOR COMMUNITY WORD)
After mother and baby went home, two nurses visited each day –– one to see the mother and one to see the baby.
“A nurse came to see me each day to check to be sure all was OK, there was no (postpartum) depression and that I had enough help,” Sommerville said. “The second nurse came to check on the baby, to be sure nursing was going OK and see how the baby was sleeping.”
Those daily home visits by nurses continued for about three weeks.
Then, in addition, Sommerville said, the French government gives each family about $1,600 Euros (nearly $2,000) to help parents purchase all the baby’s needs.
“In the U.S., mothers go home exhausted and overwhelmed. Without support, that’s tough,” Sommerville said. “It’s especially tough in the U.S. for single mothers who may not have family support.”
In response to Americans who denigrate the French system and call it socialized medicine, Sommerville counters, “In France, they recognize the best thing they can do for the country is invest in the future. The whole country understands how important that is. You can either pay now or pay later. The cost and expense of babies is recognized as a cost that makes France better.”
Dr. Rahmat Na’Allah, UnityPoint Health, said Peoria has one of the highest pre-term and low-birth weight rates in Illinois. Pre-term and low-birth weight are correlated with increased rates of learning disabilities.
“There is a reason why the United States has one of the highest maternal and infant mortality rates of all the developed countries,” Na’Allah said, citing the lack of support pre-conception, prenatal and infant care after delivery.
Na’Allah had her first child in Canada while her husband was in graduate school. After mother and infant left the hospital, a nurse visited them daily at home for five weeks.
Many of the patients Na’Allah sees in her obstetrics and gynecology practice have no more than six-weeks of maternity leave from their jobs. Many other countries provide six-months of paid maternity leave.
“If we want better outcomes, we have to invest in babies and families,” Na’Allah said. “That is not socialism. It’s just common sense.”
Jamille Fields Allsbrook, director of women’s health and rights at the Center for American Progress, said other countries pay less for medical coverage yet they have better health outcomes.
“Preventive care is always cheaper. The cost of a complicated pregnancy costs society more,” Fields Allsbrook said, noting there are also the moral issues of letting Black and Indigenous women suffer maternal death rates at three to four times that of white women.
These high maternal mortality rates are due to multifaceted causes. Coverage is insufficient. Women’s health care is stigmatized. Racism is a health risk. There is inadequate understanding in medical schools for cultural differences among white and minority women.
“Tackling racism in health care means training providers to listen. They are more likely to ignore women’s pain,” Fields Allsbrook said, noting that in France there is coverage for midwives and doulas – both providing more culturally competent care among some groups of women.
A recent Kaiser Family study found that Black and Brown women in the United States forego medical care more often due to concern about cost.
Maternal mortality is generally rare for the overall population but not for Black and Indiginous women. They have been dealing with high mortality for decades, and the problem is just beginning to be recognized. Maternal mortality and severe morbidity have been increasing among minority populations in recent years.
According to statistics from the Centers for Disease Control and Prevention, about 700 women die each year in the United States due to complications from pregnancy and delivery. An additional 50,000 each year have severe health consequences, both short and long-term, due to pregnancy and labor.
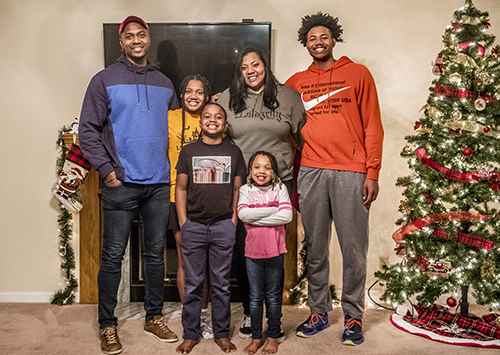
From left, Marcellus Sommerville and children Londyn, Lawson, wife Brooke, daughter Liberty and son Lathan. (PHOTO BY DAVID ZALAZNIK FOR COMMUNITY WORD)
