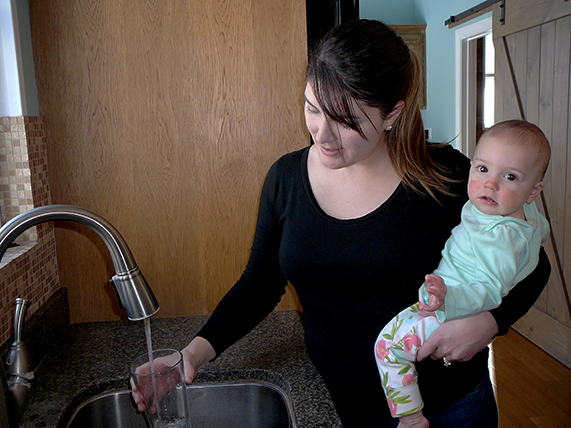
Holding her 8-month-old daughter Tahlia, Tiffany Cruse runs water from her kitchen faucet, the same faucet she uses to take water samples for testing. Cruse is a member of the Morton “Water Warriors.” (PHOTO BY ANDREA ROTH)
BY ANDREA ROTH
When Morton resident Tiffany Cruse takes her 8-month-old daughter Tahlia, for a medical checkup, she’s asked about lead paint.
“What’s concerning to me is it’s (questions) only about paint, not other sources (of lead poisoning). I know I don’t have lead paint,” Cruse said. “I also don’t have lead pipes in my house, but I still have lead in my water.”
Concern over lead paint isn’t new, but for many, myself included, our drinking water is a newer concern. I regularly meet with other moms to discuss health challenges like water. We call ourselves the “Water Warriors” because pure water is so important. According to Public Act 099-0922, all Illinois schools built before Jan. 1, 1987, were required to test for lead in 2017. Schools built between Jan. 2, 1987 and Jan. 1, 2000 must complete lead testing by the end of 2018.
“People have a right to know what’s in their drinking water and this (mandated school testing) will help them know about this one significant threat,” said Kim Knowles, of the Prairie Rivers Network, who helped draft the legislation. “It is extremely damaging for babies and children. There are lasting, lifelong effects from lead.”
While tasteless and odorless, lead is cumulatively stored in bones, organs and tissues. Lead paint, ceramic dishware, vinyl mini-blinds, hobby materials and other consumer products all contribute to child and adult lead burdens. Adults working where lead dust is prevalent, like firearm ranges, also can expose children and themselves to lead on clothing. For adults, lead can cause neurological, kidney, heart and reproductive complications.
“I know lead is stored in your bones, so I’m now wondering about nursing Tahlia because I drink a ton of water,” Cruse said.
Her home is one of 63 lead and copper sample sites in my town of Morton, and she was understandably confused about her November 2017 lead report. According to current regulations, utilities aren’t required to share copper information. Her report on lead content explained zero parts per billion (ppb) is the goal. The report stated that water filters would only be provided for homes testing over 15 ppb for lead.
“So to me that’s saying my water’s OK if the lead is less than 15 ppb,” Cruse said. “When you have public water, you assume it’s safe and if it’s not, you would know. Maybe that’s naïve. But if problems are going on, I don’t know to fix them on my end unless someone shares information. Not that they don’t want to fix problems, but it’s complicated and expensive to fix these problems and the only communication I get is this confusing letter.”
An Illinois Environment Protection Agency (IEPA) representative, Kim Biggs, agrees 15 ppb is not the health standard for lead.
“I can’t speak to how [15 ppb] was set. It’s been in place for quite some time,” Biggs said. “As we were looking at introducing legislation for schools and daycares, we did lower it for notification to parents.”
If a school’s drinking water tests at or above 2 ppb, parents and guardians must be notified according to the Illinois Department of Public Health (IDPH), the IEPA and the 2017 lead mitigation level in Public Act 099-0922.
“My kids aren’t in school, I just didn’t know about the new changes,” Cruse said. In 2016, her home water lead level was 4.2 ppb, and in 2017, it was 1.3 ppb.
According to Dr. Jerome Paulson, American Academy of Pediatrics’ Medical Director for the Pediatric Environmental Health Specialty Units – East, the 15 ppb EPA requirement was never health based.
“The real message is that 15 ppb is a standard that’s meaningless, the real goal is zero ppb, period,” Paulson said. “15 ppb was derived from an engineering standard, and they thought it would be relatively easy to get the lead lower than 15 ppb. From an engineering and cost standpoint it would be difficult to comply if the standard was lower than 15ppb.”
The health concern is that younger children are more at risk for lead poisoning due to their size and how much lead they absorb.
“Kids under age 2 will absorb 50 percent of the lead they ingest. Older teenagers and adults only absorb about 10 percent of the lead they ingest,” Paulson said. “So younger kids are more likely to get an increase in their blood lead level as a result of the same exposure.”
In 2012, at the request of a medical committee, the Centers for Disease Control and Prevention reduced the “blood level lead concentration of concern” in children from 10 micrograms per deciliter to 5 micrograms. In 2016, the American Academy of Pediatrics (AAP) took an extra step and asked for new federal standards defining and testing for lead hazards in house dust, water and soil. It urges schools and child care facilities to ensure water lead concentrations do not exceed 1 ppb. According to the AAP, even blood lead levels less than 2.5 micrograms can cause lower IQ scores, impulsivity, aggression and hyperactivity in children.
When Morton elementary schools’ results were released in 2017, all water fountains listed “None Detected” (ND). This was misleading to me, given the unlikely possibility of zero ppb lead. The sampling company, Ideal Environmental, did not respond to my interview requests. One month after my formal request, District 709 released the revised reports with the water fountain data. A lead mitigation statement published Feb. 1, 2018 on District 709’s website stated, “No drinking fountains were affected,” however, the revised reports show lead present in every water fountain previously labeled ND. Three of the four Morton elementary schools each had two water fountains testing over 1 ppb, and one school had seven fountains testing over 1 ppb of lead.
Justin DeWitt, chief of general engineering at IDPH, explained why some schools included no data for water fountains.
“The IDPH worked with the IEPA. They established the criteria, and the IEPA said [all labs] could test to 2 ppb. But it doesn’t mean all labs can’t test below that number,” DeWitt said. “The statue didn’t provide any guidance, but if you’re able to report to a lower number, you owe it to your client to share that number. This is so parents can tell their child, ‘Don’t drink out of that water fountain.’ Schools should want to know if they have any levels of lead at all.”
DeWitt said schools are treating higher sources immediately, but the 2 ppb standard could change in the future.
One sampling challenge is how lead interacts within public water lines and private plumbing. While lead piping was banned in 1986, public utilities without lead service lines or pipes still used lead solder and lead fittings with copper piping or other materials. Lead also can leach out of fixtures, especially brass, as lead was still allowed in water fixtures until 2014 when the lead free law nationally mandated any potable water plumbing contain less than 0.25 percent lead by weight.
“We’ve advised schools until you can get a clean bill of health, and that’s testing over time, one test isn’t definitive,” DeWitt said. “This is about preventing the poisoning of children.”
According to the AAP, preventing lead exposure in young children would have substantial benefits, saving more than 20 million total IQ points among U.S. children and billions of dollars in health care costs. When unfunded legislation changes, schools and county governments that own and operate drinking water facilities and aging infrastructures must meet new regulations at a cost to their finite budgets.
“What is the cost for taking lead to zero ppb? I want to be closer to zero ppb if I can, but do I ever think we will ever get to zero? No. What’s the fundamental issue? And it’s every community — we don’t have money. Where is the money going to come from?” said Morton Public Works Director Craig Loudermilk. “Number one is to provide safe, reliable drinking water that meets regulatory standards, but I don’t control those standards. I don’t want to put money in it if it’s going to change in 20 years. We’re looking at many future regulatory requirements, and I’ve got to plan for those things.”
But who pays the highest cost when regulations don’t meet health standards? The cruel irony is the regulatory system is currently set up so improvement happens only when consumers speak out, are injured or die as a result of water problems, as with Illinois’ Legionnaire’s outbreaks.
While Morton has primarily copper piping throughout the village, three homes recently exceeded 36 ppb for lead, 34 other homes were between 1 ppb and 8 ppb. Loudermilk said one sampler tested an infrequently used upstairs sink, which he thinks caused a lead spike. In 2016, the U.S. EPA began reviewing revisions for its Lead and Copper Rule (LCR), including clarification and strengthening current sampling requirements. Dr. Ronnie Levin of the Harvard School of Public Health, Water and Health Program, explained that the current LCR allows wide discretion with sampling methods.
“For example, give a consumer a narrow neck bottle and they have to run the water slowly, which brings water out of the middle of the pipe, not the edges where the metal is,” Levin said. “But whether the lead comes out and how much is a function of how corrosive the water is. And only the water utility can change [corrosiveness], you can’t change that. It’s a complicated rule.”
Levin cautions consumers about potential lead spikes anytime corrosive water sits for hours.
Unlike lead, copper is an element needed for health; however high copper is also toxic with excessive accumulation leading to brain fog, chronic fatigue, adrenal and hypothyroid issues, depression, panic attacks and more serious issues depending on exposure.
“It’s based on the Goldilocks principle,” said Paulson. “You don’t need very much copper, you need some, but the concern is you could, at least hypothetically, get too much from drinking water.”
In 2016, Morton exceeded the EPA guidelines for copper in wastewater, so testing sites were doubled. Then, Morton exceeded copper in drinking water at 2.9 mg/L; the EPA copper action level is 1.3 mg/L. Morton must now test for lead and copper every six months, instead of once every three years. I learned of Morton’s high copper in May 2017 when a fellow Water Warrior had her water tested. Her copper levels were at 4.52 mg/L. EPA action exceedance levels for copper and lead mean the public utility must take steps to reduce corrosive water.
My fellow water warrior and I called the IEPA, and met with Loudermilk and the mayor regarding our concerns. We learned EPA guidelines do not require public utilities to notify residents of high copper. Morton held a public meeting in June 2017 regarding the high copper. About a dozen residents attended, but my friend and I were the only two who spoke. For over 14 years, Morton has paid the engineering consultant company, Crawford, Murphy and Tilly (CMT) to provide EPA and water guidance. Teresa O’Grady of CMT detailed the copper exceedance and said the Morton corrosion control plan will continue through 2021. Morton is now at 1.2 mg/L for copper, just under the EPA action level.
“I think anytime consumers get involved is good, that’s not just water treatment, that’s everything. I’ve only got so much time,” Loudermilk said. “If I can get 100 people in the room then I will exert the energy. But when two or three people show up, how much time do I invest in it if no one cares?”
Because current Illinois law also doesn’t include a strict penalty or public notification process when schools or cities have water issues like high copper, public pressure is the primary incentive for change.
“Sharing more information makes things more complicated on their end, but it’s their responsibility,” Cruse said. “I’m told the water is my responsibility, since it goes through my home, but it’s their water. In the end it seems like no one is taking responsibility for our water because everyone thinks someone else is taking care of it. It’s a vicious cycle.”

2 comments for “Morton Water Warriors”